Understanding Prostate Health
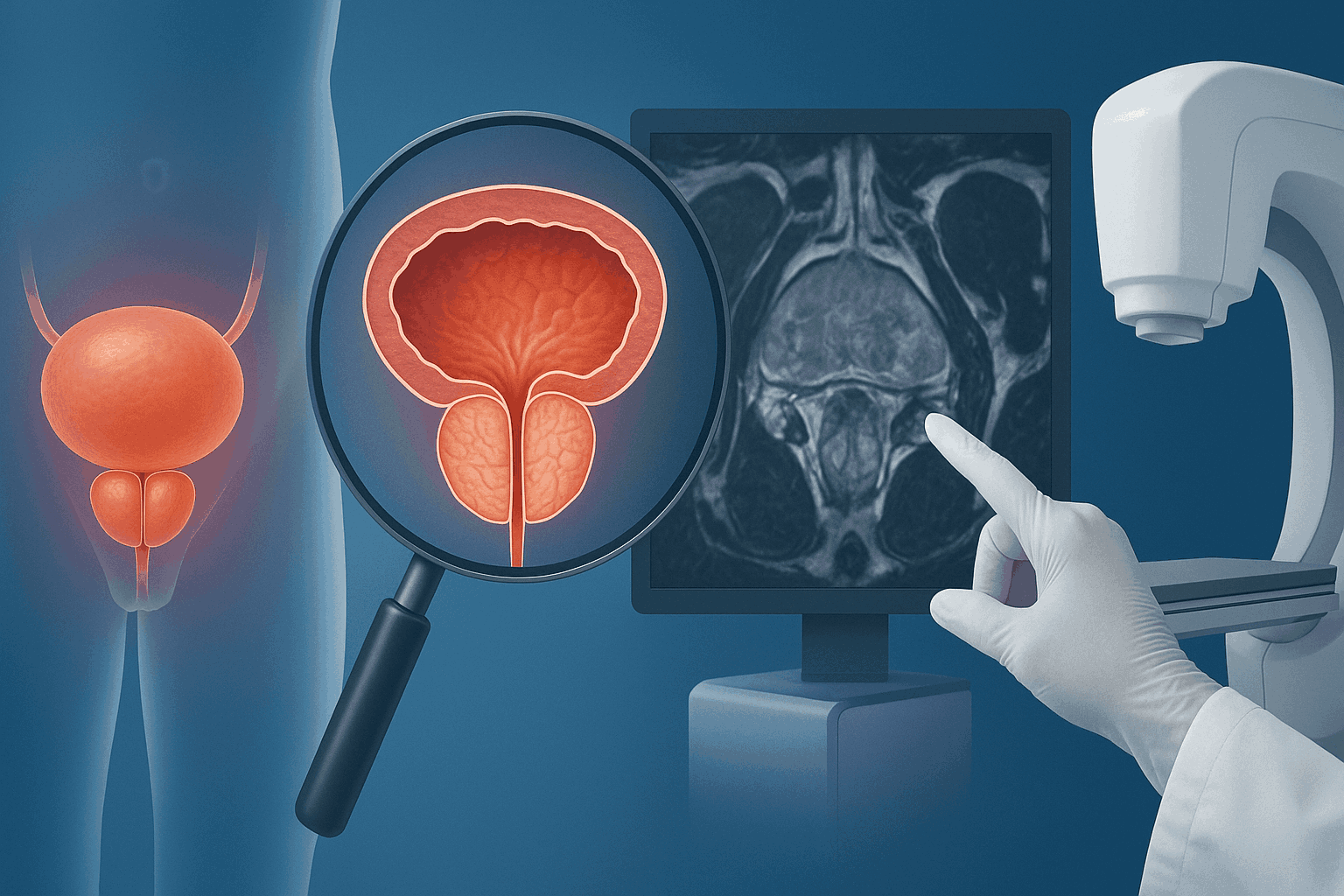
Prostate health is an essential part of men’s overall well-being, yet it’s often overlooked until symptoms appear. The prostate gland—a small walnut-sized organ located below the bladder and in front of the rectum—plays a vital role in male reproductive health by producing seminal fluid that nourishes and transports sperm.
Like any other organ, the prostate can experience various conditions, including prostatitis (inflammation of the prostate), benign prostatic hyperplasia (BPH) (enlargement of the prostate), and prostate cancer. Each of these conditions can cause lower urinary tract symptoms (LUTS), which often overlap, making medical evaluation crucial for an accurate diagnosis.
Common Prostate Symptoms
Early symptoms of prostate-related issues may seem mild but should never be ignored. Men experiencing any of the following prostate symptoms should seek medical attention:
- Difficulty starting or stopping urination
- Weak or interrupted urine flow
- Frequent urination, especially at night
- Pain or burning during urination
- Blood in urine or semen
- Discomfort in the pelvic area or lower back
- Painful ejaculation
While these symptoms can indicate benign conditions like prostatitis or prostate enlargement, they can also be early signs of prostate cancer—which often develops silently in its early stages.
Prostate Cancer: A Silent Threat
Prostate cancer is one of the most common cancers among men worldwide. It occurs when abnormal cells in the prostate multiply uncontrollably. The risk increases with age, family history, and certain genetic factors, particularly BRCA2 mutations. Men with BRCA2 prostate cancer often develop the disease at a younger age and may have more aggressive forms of cancer.
Despite these risks, prostate cancer has an excellent survival rate when detected early. That’s why regular screening and proactive prostate health checks are critical, especially after age 40 or earlier for those with a family history of the disease.
Early Detection: The Key to Better Outcomes
1. PSA Test
The PSA test (Prostate-Specific Antigen test) is a simple blood test that measures the level of PSA—a protein produced by the prostate gland. Elevated PSA levels can indicate prostate problems such as prostatitis, benign enlargement, or prostate cancer.
However, a high PSA doesn’t always mean cancer. Factors like infection, recent ejaculation, or even bicycle riding can temporarily elevate PSA levels. That’s why a doctor will interpret your results alongside your clinical history and other findings.
2. Prostate Exam
A prostate exam, also called a Digital Rectal Exam (DRE), is a quick physical examination where the doctor feels the prostate through the rectal wall to check for any hard areas, lumps, or irregularities. While mildly uncomfortable, it’s an essential part of early cancer detection.
3. Prostate Imaging
If your PSA or exam results are concerning, advanced imaging such as Multiparametric MRI (mpMRI) may be recommended. This technology helps identify suspicious areas within the prostate and guide targeted biopsies.
4. Prostate Biopsy
A biopsy is the only way to confirm prostate cancer. Tissue samples are examined to determine if cancer is present and how aggressive it is, usually graded by the Gleason score.
2023 AUA/SUO early detection guideline:
“The 2023 AUA/SUO guideline recommends offering prostate cancer screening every 2–4 years for men aged 50–69, with personalized decisions based on risk, PSA level, and shared decision-making.”
Risk Factors for Prostate Cancer
Several factors increase the likelihood of developing prostate cancer:
- Age: risk rises steadily after 50.
- Family history: a father, brother, or son with prostate cancer increases your risk.
- Inherited genes: especially BRCA2. Men who carry BRCA2 variants face a higher likelihood of developing BRCA2 prostate cancer, often at a younger age; many experts recommend earlier PSA testing in these men (commonly starting at 40).
- Ethnicity: some populations have higher risks and different disease patterns.
- Lifestyle factors: body weight and activity level may influence risk and outcomes.
At Medeor Hospital Abu Dhabi, our urology specialists recommend annual screening from age 50—or age 40 for men at higher genetic risk.
Diagnosis and Staging
Once a prostate biopsy confirms cancer, additional tests help determine how far it has spread (staging). These may include MRI, CT scan, or bone scan. Staging helps doctors design a personalized prostate cancer treatment plan.
The cancer is graded based on the Gleason score, which assesses how abnormal the cells look. A higher Gleason score means more aggressive cancer.
Prostate Cancer Treatment Options
Treatment depends on the stage of cancer, patient’s age, general health, and personal preferences. At Medeor Hospital Abu Dhabi, our multidisciplinary oncology team tailors treatment to each patient’s needs.
1. Active Surveillance
For low-risk or slow-growing cancer, immediate treatment may not be necessary. Doctors closely monitor PSA levels, repeat MRIs, and perform periodic biopsies to ensure the cancer isn’t progressing. This approach minimizes unnecessary side effects.
2. Prostate Surgery
Prostate surgery (Radical Prostatectomy) involves removing the prostate gland and surrounding tissues. It can be performed via open surgery, laparoscopy, or robotic-assisted techniques. Surgery offers excellent outcomes for localized cancers but may temporarily affect urinary control and sexual function, which can be managed through rehabilitation and therapy.
3. Radiation Therapy
Radiation therapy uses high-energy rays to destroy cancer cells. It’s a non-surgical option for localized or locally advanced cancer. Modern techniques precisely target the prostate to minimize side effects.
4. Prostate Laser Treatment
In selected cases, prostate laser treatment or focal therapy can be used to remove or destroy small cancerous areas without removing the entire gland. This approach can preserve urinary and sexual function in eligible patients.
5. Androgen Deprivation Therapy (ADT)
Androgen deprivation therapy—also known as hormonal therapy—reduces testosterone levels or blocks its action, since prostate cancer cells depend on male hormones to grow. ADT may be used alone in advanced cases or combined with other treatments like radiation for better control.
6. Chemotherapy and Targeted Therapy
For aggressive or metastatic cancers, chemotherapy and novel targeted agents are available. In BRCA2 prostate cancer, targeted therapies such as PARP inhibitors have shown promising results by attacking cancer cells with specific DNA repair defects.
Managing Side Effects and Recovery
Each prostate cancer treatment comes with its own potential side effects, but advancements in technology have greatly reduced their impact.
Common post-treatment considerations include:
- Urinary Control: Temporary leakage can improve with pelvic floor exercises and time.
- Sexual Health: Erectile dysfunction may occur but often improves with medications or therapy.
- Hormonal Changes: Androgen deprivation therapy can cause fatigue, mood changes, or hot flashes, which can be managed with medical and lifestyle support.
At Medeor, post-treatment care includes physiotherapy, nutritional guidance, and mental health support to ensure holistic recovery.
Prostatitis vs. Prostate Cancer
It’s important to understand that not all prostate conditions are cancerous. Prostatitis, for instance, is an inflammation of the prostate that can mimic cancer symptoms. It often presents with pelvic pain, painful urination, or fever. A thorough medical evaluation—including a PSA test and imaging—helps distinguish between these conditions.
Frequently Asked Questions (FAQs)
1. When should men start screening for prostate cancer?
Men should begin discussing PSA testing and prostate screening with their doctor at age 50. Those with family history or BRCA2 mutations should start at age 40.
2. Does a high PSA level always mean cancer?
No. Elevated PSA can result from prostatitis, benign enlargement, or even recent sexual activity. Your doctor will consider multiple factors before suggesting a prostate biopsy.
3. How is prostate cancer confirmed?
Through a prostate biopsy, tissue samples are examined for cancer cells. Imaging tests further help in determining the stage.
4. Is prostate cancer curable?
Yes, especially when detected early. Localized cancers can often be cured with prostate surgery, radiation, or laser treatment.
5. What are the side effects of androgen deprivation therapy?
Androgen deprivation therapy can cause reduced libido, fatigue, and bone loss, which can be managed through medication, exercise, and dietary changes.
6. Can lifestyle changes prevent prostate cancer?
While not completely preventable, maintaining a healthy weight, exercising regularly, and eating a balanced diet rich in fruits and vegetables can support better prostate health.
7. What is BRCA2 prostate cancer?
It’s a hereditary form of cancer caused by mutations in the BRCA2 gene, often requiring earlier screening and sometimes different treatment strategies.
8. What’s the difference between prostate laser treatment and surgery?
Prostate laser treatment is minimally invasive, and targets only affected tissue, while prostate surgery removes the entire gland. The right option depends on cancer stage and overall health.
9. How often should I take a PSA test?
If your PSA is normal, once every 1–2 years is recommended, depending on age and risk factors.
Q10. Can prostate cancer come back after treatment?
Yes, recurrence is possible, which is why ongoing PSA monitoring and follow-up appointments are essential for long-term care.
Conclusion
Prostate cancer is a disease where early awareness truly saves lives. By paying attention to prostate symptoms, staying informed about your prostate health, and undergoing timely screening through PSA tests and prostate exams, you can detect issues early—when they’re most treatable.
At Medeor Hospital Abu Dhabi, our multidisciplinary team of urologists, oncologists, and specialists offers comprehensive prostate cancer treatment—from advanced diagnostics and minimally invasive prostate surgery to personalized androgen deprivation therapy and prostate laser treatment. We combine medical excellence with compassionate care to help every patient achieve the best possible outcome.
Prioritize your prostate health today
If you’re experiencing urinary symptoms, have a family history of prostate cancer, or are over 40, schedule your PSA test or prostate exam at Urology Department of Medeor Hospital Abu Dhabi.
Your health is worth every early step—because early detection makes all the difference.